Keratoconus is a degenerative eye condition resulting in the thinning and protrusion of the cornea, the clear, dome-shaped front part of the eye. This abnormal shape prevents light from focusing inside the eye correctly, distorting vision.
An irregular corneal shape can lead to various symptoms, including blurry vision, light sensitivity, and glare. Both eyes can be affected by keratoconus, but it’s common for one eye to be worse than the other. Various corrections and treatments for keratoconus exist, from specialty contacts to cornea replacement surgery.
Typically, Keratoconus begins during late adolescence or early adulthood, with symptoms progressing gradually over a period of 10 years or more. This is one of the many reasons taking your child for regular eye exams is vital—early diagnosis can help set them up for years of healthy vision.
The Importance of Treating Keratoconus
Treating keratoconus early helps prevent vision loss and improve quality of life. A specialized eye doctor should be consulted to determine the best course of treatment for your individual case.
Common symptoms include frequent changes in eyeglass prescriptions and sudden worsening or clouding of vision. In some cases, the cornea may swell, severely impacting your eyesight. This happens when strain on the cornea creates a tiny crack, which may take weeks or months to heal and often scars.
If sudden swelling occurs, your eye doctor can prescribe eye drops for temporary relief. With proper treatment, many people with keratoconus can effectively manage their condition and maintain good vision. It’s important to seek immediate help if you experience symptoms of keratoconus. Seeking treatment for keratoconus at an early stage can increase the likelihood of better outcomes.
Non-Surgical Treatment Options
Contact Lenses & Eyeglasses
Mild cases of keratoconus can be corrected with eyeglasses or soft contact lenses. But as this condition advances, these traditional methods may not be enough. Your optometrist may recommend specialty contacts custom fit for your eyes.
Specialized lenses like rigid gas-permeable contacts or scleral lenses can help address the condition. These lenses provide a more precise fit, better visual acuity, and improved clarity and comfort for those with keratoconus.
Prescription Eye Drops
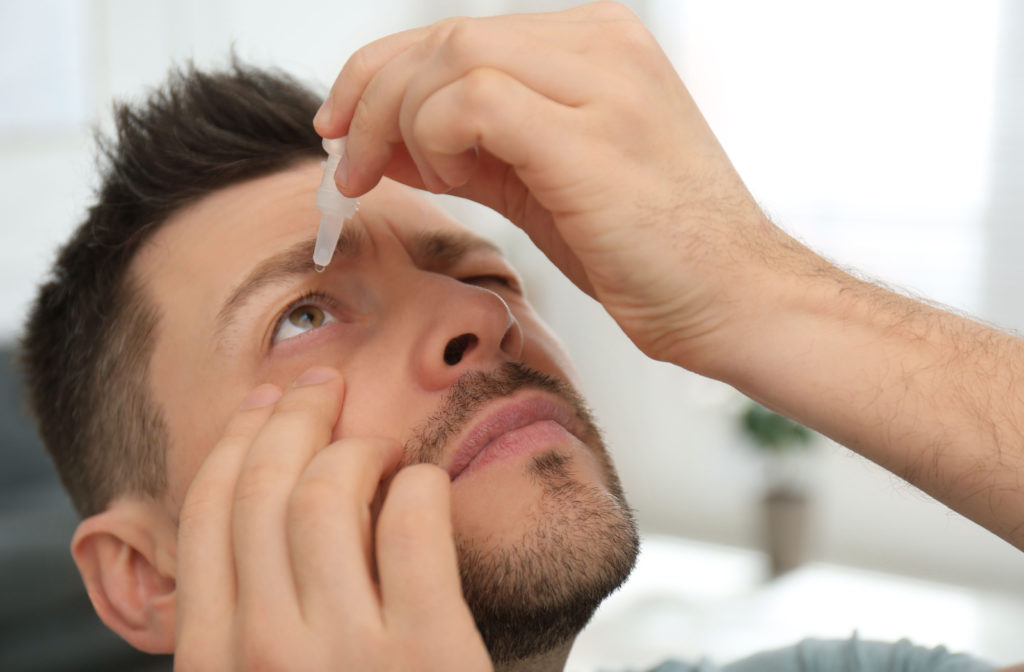
If you experience a sudden bulging of your cornea, your doctor may prescribe eye drops to relieve your symptoms temporarily. These drops don’t stop the underlying condition or fix your cornea, but they can significantly slow the progression of keratoconus.
Medications that improve metabolic processes in the cornea, such as taurine, dialysate, and retinol acetate or vitamin A, may be included in the drops.
Intacs
Intacs are small, curved, and transparent plastic devices implanted into the cornea to correct vision problems over a long period. This innovative medical technology is part of the intrastromal corneal ring segment (ICRS) family and primarily treats eye conditions such as keratoconus.
Intacs can help alleviate the symptoms of keratoconus and improve visual acuity, allowing patients to enjoy a better quality of life.
Surgical Treatment Options
Corneal Cross-Linking
Corneal collagen cross-linking can help treat keratoconus. This procedure can slow or even stop the condition’s progression, potentially avoiding the need for a cornea transplant in the future. It’s recommended to have the surgery early after diagnosis, but it can also be helpful later on if your eyeglass prescriptions continue to worsen.
It’s minimally invasive and strengthens the collagen bonds in the cornea, making it stiffer and preventing it from bulging out.
Corneal Transplant
If your condition worsens, you may need a cornea transplant. Typically, corneal transplants are performed as an outpatient procedure and take about an hour.
During the surgery, the patient’s cornea is removed, and a donor cornea is carefully sewn into place using tiny stitches that usually stay in for more than 12 months. After the transplant, vision may remain blurry for several months.
Medication must be taken continuously to prevent rejection of the transplanted tissue, including anti-inflammatory eye drops. In almost all cases, glasses or contact lenses are still needed to achieve clear vision after corneal transplant surgery.
Choosing the Right Treatment
Choosing the right treatment depends on the severity of keratoconus, your preferences, and weighing each procedure’s potential risks and benefits.
Your optometrist or ophthalmologist will review your options and let you know which treatments best suit your condition.
If caught early enough, contacts and glasses may be your best option. But as the issue worsens, more invasive procedures may be necessary to improve your vision.
Contact us at Pacific EyeCare Optometry. We’re here to help you every step of the way. Book an appointment with us today!



